Schools Earn Poor Marks When It Comes to Kids’ Mental Health
A coalition of mental health advocacy organizations released a report card, rating each of the 50 states and Washington, D.C. on their school mental health policies. The group didn’t give out grades, but if they did, there wouldn’t be any As.

Updated to add chart of state-by-state rankings.
The pandemic may have exacerbated the mental health crisis in the nation’s children, but it certainly didn’t create it.
Kate, a former adolescent therapist, said her son was 7 when he first began exhibiting attention issues. By early 2020, when he was in fifth grade, he had two diagnoses – generalized anxiety disorder and attention deficit hyperactivity disorder – both of which were shared with his school. Yet he still found himself being routinely banned from recess for acting out in class.
“Some of his problems in the classroom, like sitting still and impulse control, stem from being anxious in that environment,” she told Mindsite News. Like many educators, the boy’s teacher was not trained to deal with kids with mental health issues, Kate said. She asked that she be identified by her first name only and that her son’s name be withheld.
The problems faced by Kate’s son are far from unique. Today, a coalition of mental health advocacy organizations released America’s School Mental Health Report Card, rating each of the 50 states and Washington, D.C. on a range of school mental health policies. The group didn’t give out grades, but if they did, there wouldn’t be any As, and only seven states scored 50% or higher.
In the report card, each state is graded from 0 to 3 on each of eight policy categories ranging from how well teachers, staff and students are trained and taught about mental health concepts to the ratio of mental health professionals to students. Other key metrics include how safe and inclusive the school’s climate is, the extent of partnerships between schools and the community, and whether students are regularly screened for depression or substance abuse.
The seven states at the top of the rankings – those scoring 12 to 14 out of a possible 24 – are Colorado (14), Illinois (13), Nevada (13), Washington (13), Maryland (12), New Hampshire (12) and North Carolina (12). Six states scored 5 or under: South Dakota (3), Nebraska (4), New Mexico (4), Wyoming (5), Montana (5) and Alabama (5).
How states rank in school mental health ratings
A coalition of mental health advocates ranked states on how well they are doing at ensuring that public schools look out the mental health of students. Here are their rankings:
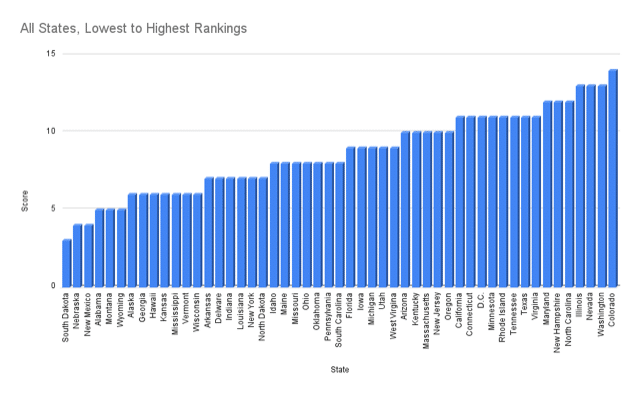

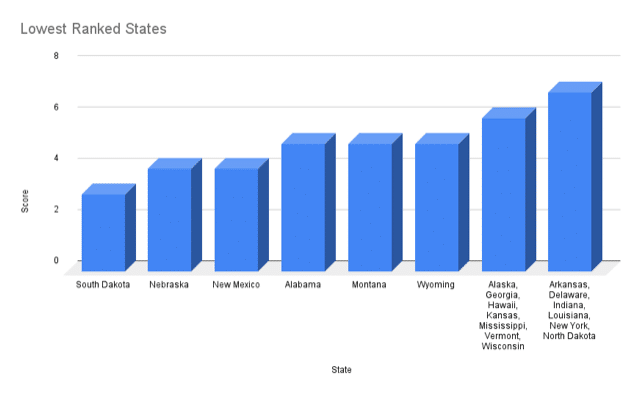
Data compiled from America’s School Mental Health Report Card
“Our research reveals that there are enormous gaps in every state, which are leaving our children shortchanged,” said Angela Kimball, senior vice president for advocacy and public policy at Inseparable, the national mental health nonprofit that led the ratings effort. But their investigation also found “surprising amounts of innovation,” she said.
One of the innovators is Maryland, which scored 12 of 24 in the ratings. In recent years, the state’s education code has called for “restorative approaches” to be used in all schools.
“Restorative practices have two sides: one is proactive, the other responsive,” and both aid students’ mental health, said Kathryn Rockefeller, a school climate specialist for Anne Arundel County Public Schools in Annapolis.
On the proactive side, Arundel schools allocate time for building relationships among students and staff. Once a day in elementary schools, students sit in a circle with their teacher, who has been trained in the program. A talking stick handed around allows each student to speak – or pass – while others actively listen to the question of the day.
“Developing empathy and taking turns speaking are such important skills,” Rockefeller said. The program is used less frequently in older grades, she said, and seems to be less effective.
The reactive side aims to teach life skills and resolve conflicts, without resorting to suspensions or expulsions – which nationwide tend to be disproportionately levied against students of color and those with mental health needs. Kids who fight, vandalize, or otherwise misbehave are immediately asked five questions including what they were thinking, what others involved might have been thinking, and how they can make the situation better. Then they’re asked to attend a “responsive circle” with all parties to reach a resolution.
“We are not punishing students but teaching them things like how to resolve conflicts or that you get power by owning your responsibility,” Rockefeller said.
One in three feeling sad and hopeless
Even in 2019, the year before COVID-19 swept the world, more than one in three high school students experienced persistent feelings of sadness or hopelessness, and one in six young people considered suicide, according to the U.S. Centers for Disease Control and Prevention (CDC).
Roughly half of children with mental-health conditions get treatment for it. If only half the kids with diabetes were being treated, we would be appalled.”
Angela kimball
Two years of lockdowns, loneliness, lack of support – and, for some kids, the loss of a loved one – put mental health on the radar for parents and the public. Rates of anxiety and depression among children doubled after the pandemic started, prompting the American Academy of Pediatrics to declare a national state of emergency in child and adolescent mental health.
But despite increased awareness, the report makes clear that youth aren’t getting the resources they need. “Roughly half of children with mental-health conditions get treatment for it,” said Inseparable’s Kimball. “If only half the kids with diabetes were being treated, we would be appalled.”
Mental health advocates consider schools the best place to provide mental health supports to children. “Kids are in school so much of the day, so the responsibility naturally falls on the schools,” Kimball said.
Last December, a Fairfield, Connecticut, mother discovered that her depressed 12-year-old son was searching online for methods of committing suicide and immediately called the school. It took several days before a guidance counselor spoke with him, and there was no follow-up. The boy is seeing private mental health clinicians, but his mother worries about those who can’t afford to do the same. “So many kids are in crisis now. Schools don’t have the resources to address what’s going on,” she said.
Report Card Provides a Roadmap

The report represents an effort by Inseparable and more than a dozen nonprofit groups, including the National Alliance on Mental Illness and the Healthy Schools Campaign to assess states’ performance and create a coalition – the Hopeful Futures Campaign – that can prod both federal and state policymakers.
The groups are working to “to better support schools in doing this work,” said Alex Mays, senior national program director at the Healthy Schools Campaign. Billions of federal Covid relief dollars going to schools makes funding new programs easier, she said.
Parents are demanding change, too. A recent online survey by the Harris Poll conducted on behalf of Inseparable found that 87 percent of adults are concerned about youth mental health in the U.S.
The report card provides a comparative framework so each state can see how well it is doing compared with others. It also highlights specific leading-edge programs the group hopes other states follow.
Many parents would like to see more training for teachers in mental health, said Kate, the former therapist, who now coaches families of children with mental health concerns. “A lot of parents tell me their child is labeled ‘the bad kid’ or ‘the destructive kid,’ even though their brains are not capable of changing their behaviors,” she said. “Parents of these children feel frustrated and misunderstood.”
One metric where nearly all states fall short in the report is the number of mental health professionals a school has on staff. The National Association of School Psychologists recommends one psychologist for every 500 students. Only the District of Columbia and Idaho reach that goal. By contrast, Alaska and Georgia have ratios of more than 1 to 5,000.
A number of states do better in creating school-family-community partnerships, such as a new Texas program that offers a model to other states, Kimball said. In 2019, the state legislature created a consortium of psychiatry departments from 13 medical schools and other health institutions that is tasked with helping provide mental health care to K-12 students, including via telehealth.
The state is now rolling out a program called TCHATT that provides students up to five free video telehealth appointments, held during the school day. It’s an important way to deliver services in a large state like Texas, said Laurel Williams, D.O., the consortium’s medical director. “Families in rural areas can spend hours in the car accessing mental health,” she said.
Texas does not seek Medicaid reimbursement for the telehealth services, even though the law allows it. That means the state is leaving federal money on the table if they don’t bill the program for work in schools, said Mays. “In order to really expand access to school mental health, there needs to be sustainable funding,” she said.
Sometimes Counties Take the Lead
In some states, counties are instituting mental health policies on their own, even when the state doesn’t require it. Indiana, for example, scores only 7 of 24, but the county of Tippecanoe offers a number of programs including aggression replacement training (ART) – aka anger management – to kids who act out.
The six-week program helps students “learn to recognize what triggers their anger, the cues their body gives them when it’s starting to rise, and the coping skills like deep breathing to calm themselves,” said Maddie Riordan, the county school services director. Students who have been through the training are no longer as disruptive in the classroom, she said.
Without these services, he probably would have given up and dropped out,”
amy shuman
One Tippecanoe high high school student who participated in the ART program had been diagnosed with anxiety, impulsivity disorder and trauma and often fought with other students, said his stepmother, Amy Shuman. The ART training and other school-provided services have made a huge difference, she said.
She wished these services had been made available in middle school, when her son’s issues were not as severe, but is thrilled with the supports he’s getting now. “Without these services, he probably would have given up and dropped out,” she said. “With all they’re doing, I feel like the school is wanting him to succeed and graduate and thrive.”
Tippecanoe county has also trained school resource officers and police to understand teen brain development, including how mental health issues affect behavior. This national program, called Policing the Teen Brain, provides cops in schools with tools to deescalate situations on the spot, said Aaron Gilman, a county deputy sheriff and school resource officer.
Recently, teachers tried to take wheeled sneakers from a boy with emotional issues and he became agitated. Gilman sat down and had a calm conversation with the boy and in the process, gained some insight: The boy reacted as he did because his family had little money and the shoes were the one valuable object he possessed.
Seeing If the Kids Are All Right
Since students’ mental health problems often go undiagnosed, the report also looks at how well schools check on kids’ wellbeing though tool such as depression screens. “These give an early look at whether someone is struggling and can benefit from extra help,” Kimball said. This is especially important because 50 percent of chronic mental health conditions present by age 14, she said.
States are increasingly recognizing the importance of these checks. In 2021, for example, New Jersey allocated $1 million for annual depression screens for students in grades 7 to 12 (earning it a 2 out of 3 in this category).
Instituting widespread screening is challenging but doable, said E. Rebekah Siceloff, Ph.D., a research associate at the University of South Carolina who coauthored a study of a screening program in one public school district. (Such screening is not mandated by South Carolina, earning the state a zero in the category.)
Identifying students with mental health concerns is only a first step, Siceloff said. “The benefits can only be maximized if those identified students are referred for follow-up assessment and linked to appropriate mental health care and support in a timely manner,” she said.
Doing that might get you a decent grade on a school report card.
The name “MindSite News” is used with the express permission of Mindsight Institute, an educational organization offering online learning and in-person workshops in the field of mental health and wellbeing. MindSite News and Mindsight Institute are separate, unaffiliated entities that are aligned in making science accessible and promoting mental health globally.






