One in Nine Arrests Are of People with Both Mental Illness and Addiction, New Study Finds
Some 7.5 million people were arrested in the U.S. in 2020, and more than 10 million people were arrested each year in the 2010s. Now a new study looking at three of those years, 2017 to 2019, finds that one in nine of all arrests was of a person grappling with both a mental health and substance use disorder.

Some 7.5 million people were arrested in the U.S. in 2020, and more than 10 million people were arrested each year in the 2010s. Now a new study looking at three of those years, 2017 to 2019, finds that one in nine of all arrests was of a person grappling with both a mental health and substance use disorder.
Although each of these problems – mental health disorders and addiction – is considered to be a medical condition, a disproportionate number of people with these problems are cycling through jails and prisons, said Tracy Velázquez, a senior research manager at Pew Charitable Trusts and co-author of the report.
“Addressing the needs of this population could both reduce the use of the criminal justice system and improve outcomes for these individuals and their communities,” she said on a conference call with journalists following the report’s release.
At a time when policymakers are looking at ways to address and reduce the large number of people with mental illness who are incarcerated or revolving through the criminal justice system, the report suggests how strongly intertwined addiction and mental illness are.
Using self-reported data from the National Survey on Drug Use and Health, the study estimated that 60% of those arrested with mental illness have a co-occurring substance use disorder. It also found that more than one in nine adults with co-occurring disorders are arrested annually – a rate 12 times higher than adults with neither condition.
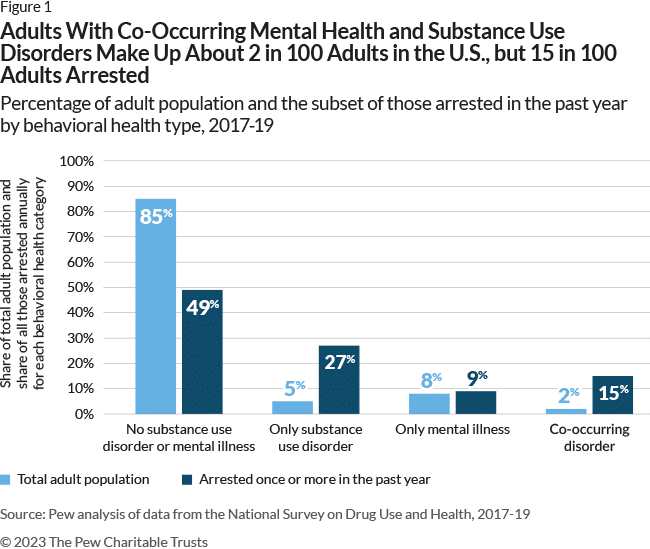
In almost half of these cases, the most serious charge against the arrested person was substance-related. Arrests damage people’s employment prospects and depress their wages, worsen their housing stability and their physical and mental health. For an already vulnerable population, each of these problems increase the likelihood of them being rearrested, according to the study.
People with one or both of these disorders are more likely to struggle with homelessness, childhood trauma, poverty and physical disorders, leaving them in situations where police are likely to be called, said Andrew Cleek, a psychologist and deputy executive director of the McSilver Institute for Poverty Policy and Research at New York University.
“Once the police are there, the options get truncated,” Cleek said. “The tools that they have are arrest, bring somebody to the emergency room, or bring somebody to jail, rather than really considering treatment in a holistic way.”
The failure of the treatment system was also clear. While research shows that treating both mental illness and substance use disorders produces the best outcomes, only 10% of adults with co-occurring disorders received treatment for both of their conditions in the past year, the study found.
Fewer than half of Black (47%) and Hispanic (43%) adults with co-occurring disorders received treatment for even one of their conditions, compared with 64% of white adults.
“The system is wholly unprepared to address the needs of individuals with mental health issues or individuals with substance use issues,” Cleek said. “But when you combine those issues the system is just not set up to provide the kind of comprehensive care needed.”

The Pew report found that people named numerous reasons for why they weren’t receiving treatment including stigma, cost, and not feeling ready to engage in treatment.
A major contributor is the growing lack of providers in the behavioral health space, including “culturally competent providers,” Velázquez said.
Cleek recommended broadening the use of new models that don’t deploy police as first responders for people with mental health and substance use needs, improving access to treatment, and creating more certified community behavioral health clinics, which provide mental health and addiction regardless of peoples’ ability to pay.
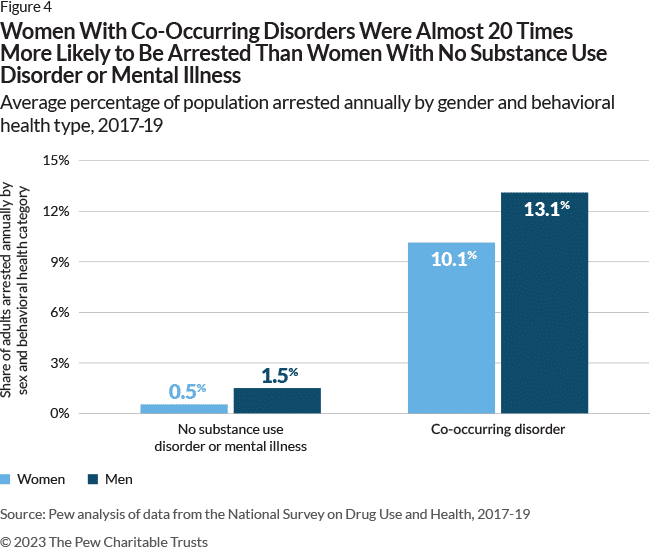
People with co-occurring disorders often report being victims of violence themselves, Velázquez said. Many, if not most, have histories of trauma. Women, in particular, are frequently victims of sexual abuse and are more likely to experience trauma at a younger age, she said.
“This all points to a need for more trauma responsive interventions to reduce arrest and incarceration,” she said. Police should “consider the potential re-traumatizing impacts of their encounters with women.”
Other findings:
- Women with co-occurring disorders were arrested 19 times more often than women with neither.
- Black adults with co-occurring disorders were arrested 1.5 times more often than white adults.
- People with co-occurring disorders involving methamphetamine had the greatest likelihood of arrest.
Providing integrated treatment for both disorders and reducing police response to social issues like homelessness and poverty could alleviate the cycle of recidivism in these populations, Velasquez and her colleagues said.
The name “MindSite News” is used with the express permission of Mindsight Institute, an educational organization offering online learning and in-person workshops in the field of mental health and wellbeing. MindSite News and Mindsight Institute are separate, unaffiliated entities that are aligned in making science accessible and promoting mental health globally.