Research Roundup: Trajectory of Depression and Tele-Mental Health’s Efficacy
The efficacy of remote mental health care appears to rank as one of the upsides to the forced social distance of the past 18 months, with higher rates of access, fewer canceled appointments, and equivalent outcomes.


This Week in Mental Health Research
Hello, readers of the Research Roundup. Good news this week for readers who want more of the stories from Psychiatric Services and have been frustrated by the paywall. We try to prioritize open-source journals for the Roundup so that you can go deeper with the original source. But some important stories from great journals like Psychiatric Services, sit behind a paywall. Lisa Dixon, editor-in-chief of Psychiatric Services, has agreed to make articles that we cover in the Roundup accessible so you can get the full story directly from the journal. We hope other journals will follow their lead. And now read on, to learn the latest research about shared decision making, telehealth, and more. And please sign up for our newsletters here.
By Tom Insel, MD
The Many Paths of Adolescent Depression
Most mental health research captures a snapshot in time. Yet mental illnesses are developmental disorders, playing out over months and years with the trajectory often being more informative than a picture at one specific moment. To understand the trajectory, we need a movie not a snapshot. The Avon Longitudinal Study of Parents and Children (ALSPAC) project has produced that movie based on data from the offspring of over 14,000 pregnant women from Avon, UK, who were enrolled in 1991 and 1992. Over more than two decades, some 2000 reports about the children of ALSPAC moms have informed our understanding of normal development, especially how genes and environment interact across adolescence.
In a new report, the ALSPAC team asks how depression during adolescence evolves over time. We know that depression frequently begins in adolescence, but some clinicians believe that these early-onset episodes of depressions are transient and don’t require treatment. It’s also possible that some forms of depression begin early and would respond best to aggressive treatment. By assessing depressive symptoms at 10 time points between age 10 and age 25, the team found four different trajectories. In one group, depression persisted across these age spans; in another it was limited to adolescence; in a third it increased moving into adulthood; and in a fourth, it remained stable at a low level.
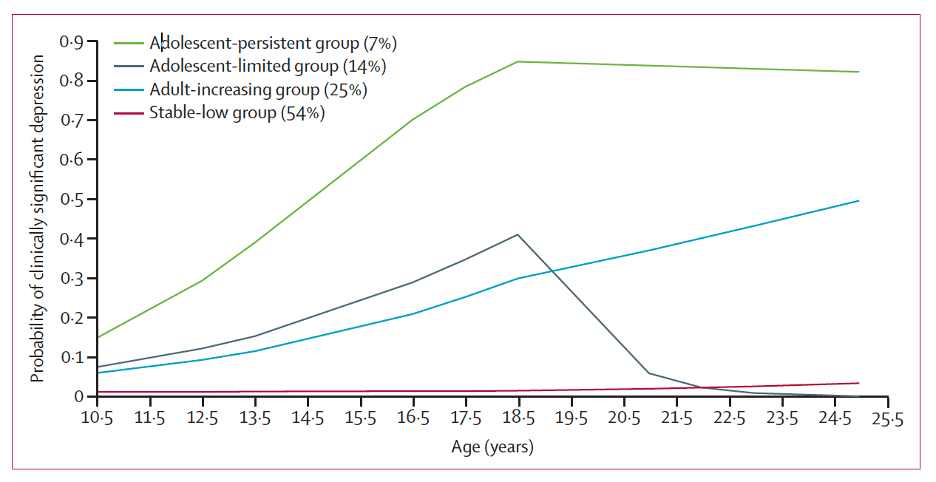
While the persistent and limited groups could not be identified (predicted?) by the symptoms or severity of depression in adolescence, their outcomes were markedly different – at least in hindsight. Kids with earlier onset, a history of adversity (poverty, adverse experiences, bullying) that persisted into adolescence, poor educational performance, and genetic loading for depression were likely to fall into the persistent subgroup. They had markedly worse mental health and occupational outcomes as adults. Indeed, 27% of this group had a history of suicidal self-harm by age 25. Conversely, those in the adolescent-limited subgroup ultimately did as well as the stable-low level of depression subgroup (only 2% of the adolescent-limited group had a history of suicidal self-harm by age 25).
We know that depression in adolescence is both common and untreated. These results point to the importance of early detection and intervention, especially for those with early and persistent depression. Studies like ALSPAC give us the picture of how mood disorders develop and when we can intervene to improve both short-term and long-term outcomes.
The antecedents and outcomes of persistent and remitting adolescent depressive symptom trajectories: a longitudinal, population-based English study The Lancet, Oct 18, 2021
Nothing About Us Without Us: Shared Decision-Making
Shared decision-making gives a person with serious mental illness a role in determining their care. This may seem like an obvious and virtuous practice, but in the real and often chaotic world of clinical care, the person with the most at stake may have little opportunity to weigh in on treatment decisions, from choice of medications to involvement of family members. In other areas of medicine, an entire industry has developed tools for educating patients and family members to facilitate communication with providers and improve decisions about care, although those decisions are generally made by the provider. In the world of serious mental illness, shared decision-making is a bit different: tools such as decision aids and advanced directives are a means to give a patient agency in critical decisions, hopefully improving engagement with care.
Does it work? Elizabeth Thomas from Temple University and her colleagues reviewed 53 studies of shared decision-making to answer that question. The answer: it’s complicated. Studies varied in the tools, the population, and the outcomes. Although some tools like CommonGround and advanced crisis planning were assessed in multiple studies, most were assessed only once. There was no consensus about what constitutes shared decision-making or how best to measure its impact. While many studies supported the idea that shared decision-making improved communication and reduced subsequent conflicts, there was surprisingly little evidence that these innovations improved treatment adherence or clinical outcomes.
There is an old saw in science: “absence of evidence is not evidence of absence.” This review, the largest to date of shared decision-making, argues for some standard approaches to determine what works. Empowering people with serious mental illness and increasing engagement with care are vital goals, essential for recovery. While “nothing about us without us” seems like it should be a fundamental ethical principle supporting empowerment and engagement, we still don’t have a scientific consensus that shared decision-making improves outcomes.
A Systematic Review of Shared Decision–Making Interventions for Service Users With Serious Mental Illnesses: State of the Science and Future Directions Psychiatric Services Nov, 2021
Telehealth for Intensive Mental Health Care? It Works.
The pandemic resulted in a massive transition from brick-and-mortar care to remote tele-mental health services. Most of the evidence suggests higher rates of access, fewer canceled appointments, and equivalent outcomes with remote care. For people with mild to moderate mental health problems, the convenience of telehealth seems to have outweighed the loss of face-to-face contact. But what about people with more severe problems?

Nyssa Z. Bulkes and colleagues from the Rogers Behavioral Health System compared outcomes for 1,192 people referred for partial hospitalization or intensive outpatient treatment during the pandemic when these intensive services were delivered by telehealth to a matched group of 1,192 people who received these same services in person prior to the pandemic. The results show that telehealth was equivalent, in terms of reduction of symptoms and improved quality of life. The only difference between the groups was a 2.8 day longer engagement in the partial hospitalization provided remotely compared to in-person.
There are not a lot of silver linings to this pandemic, but the surprising efficacy of remote mental health care appears to rank as one of the upsides to the forced social distance of the past 18 months. It is particularly surprising that intensive mental health care can be delivered as effectively by telehealth as by direct face-to-face interaction. As we emerge from this pandemic, results like these raise questions about the optimal way to deliver mental health care, particularly for people from rural, underserved populations. Will brick-and-mortar clinics become obsolete, or can we create a hybrid model that allows more options for accessing care?
Comparing efficacy of telehealth to in-person mental health care in intensive treatment-seeking adults Journal of Psychiatric Research, Nov 3, 2021
When Convenience Clashes with Risk: Suicide in the Era of the 90-Day Prescription
Most people who try to kill themselves in the US intentionally overdose on medication. In the past, getting enough pills for a lethal dose often required doctor-shopping or hoarding a supply. But this is the era of the 90-day prescription, and such supplies are now legal in every state. In 27 states, 90-day supplies are even permitted for controlled substances (like opioids).
Three-quarters of mail-order prescriptions now provide a 90-day supply. Patients appreciate the convenience, pharmacy benefit managers enjoy the savings, and healthcare providers claim improved adherence. But is it safe? While there’s no evidence yet that 90-day prescriptions have increased suicide, researchers led by Brian Barnett of the Cleveland Clinic worry that this increasingly common practice could start claiming the lives of people with mental illness.
Barnett and his team examined the impact of 90-day prescriptions on suicide risk. Several incentives fuel this trend, they found. Most perversely, some health insurers require prior authorization for short-term supplies. To avoid this requirement, providers may prescribe a 90-day supply for patients being released from a psychiatric hospital, despite the high risk of self-harm in the month following discharge. And while newer antidepressants and antipsychotics are safer than older versions, a 90-day supply can still sometimes be fatal.
What can be done? For one thing, the authors say, pharmacists should stop extending a 30-day prescription to a 90-day refill without notifying the prescriber. A “dispense-as-written” feature alone could reduce the risk for certain medications and high-risk patients. And flagging high-risk medications could help mitigate overdose.
Intentional Overdose Prevention in the Era of the 90-Day Prescription Psychiatric Services, Aug. 9 2021.
Tom Insel, MD, is a psychiatrist, neuroscientist, and former director of the National Institute of Mental Health (NIMH). He is a donor to MindSite News and chair of its Editorial Advisory Board. Dr. Insel’s financial conflict of interest statement, which includes equity and advisory roles in several early-stage mental health technology companies, can be found here.
The name “MindSite News” is used with the express permission of Mindsight Institute, an educational organization offering online learning and in-person workshops in the field of mental health and wellbeing. MindSite News and Mindsight Institute are separate, unaffiliated entities that are aligned in making science accessible and promoting mental health globally.






