Rx for Better Mental Health? M-O-N-E-Y
Money beats psychotherapy. Prevention as intervention takes a setback. Pregnant women in jail aren’t often getting treatment for their opioid disorders. And more.


January 28, 2022
By Tom Insel, MD, and Matthew Hirschtritt, MD, MPH
Good morning, Research Roundup readers. We start this week with a shoutout to all of our policy-minded readers, especially those who are thinking about how to pay for crisis services. A new report provides a roadmap for financing the continuum of crisis services (read: billing codes!). We know, it’s not research. But it’s so important for reducing incarceration and ER boarding, we couldn’t resist.
Now on to the science. For me (TI), one of my favorite papers of the past two years described an elegant study comparing cash transfers and psychotherapy among poor farmers in Kenya. A year after receiving roughly $1,000 USD, rural Kenyans had higher asset holdings and psychological well-being relative to families who did not receive cash. One year after psychotherapy there was no impact detected on either psychological or economic outcomes. And farmers who received both cash and psychotherapy – no better off than cash alone. Was this result a one-off? A new review looks at the literature, especially in low- and middle-income countries. Other studies this week examine treatment for opiate use disorder in jails, the use of digital tools to assess psychosis, the representativeness of real-world patients with schizophrenia in clinical trials, and the long-term outcomes for children receiving specialty mental health services (it’s not what you expect). Read on!
(If you like what you’re reading here, please forward this to a friend or colleague. You – or they – can sign up for our newsletters here.)
Want to Improve Mental Health of People with Low Incomes? Give Them Money

Financial hardship is frequently associated with poor health outcomes, including worse mental health, lower self-rated overall health and higher mortality. Some 6.4 billion people – more than 80% of the world population – lived in low- and middle-income countries. A new review of multiple studies suggests that giving cold, hard cash to people living in low- and middle-income countries can meaningfully increase their subjective wellbeing and mental health.
Joel McGuire of the Happier Lives Institute in Oxford, UK, and colleagues identified 45 studies encompassing about 117,000 people that examined the impact of cash transfers on subjective wellbeing and mental health among people in low and middle-income countries. They found a small but statistically significant improvement in both subjective wellbeing and mental health after an average of two years following receipt of a cash transfer. Notably, the impact of the cash transfer was strongly related to its value – both in relation to the person’s previous income and in absolute terms. There wasn’t a significant difference in outcomes following conditional cash transfers – those earmarked specifically for prespecified uses, like food – compared with outcomes following unconditional cash transfers. More money, regardless of how it was given, led to better outcomes.
This review complements and reinforces previous studies showing that cash transfers improve subjective wellbeing and mental health among youth in low- and middle-income countries. These findings are especially salient here in the U.S. as the pandemic-related child tax credit expired, effectively cutting off a financial lifeline for millions of American families with young children. Critics of financial subsidies claim that they disincentivize employment and promote an overreliance on government assistance, despite a lack of supporting evidence. McGuire’s review adds to the argument that, to improve wellbeing and mental health, cash transfers are a powerful tool.
A systematic review and meta-analysis of the impact of cash transfers on subjective well-being and mental health in low- and middle-income countries. Nature Human Behavior, January 20, 2022.
–Matthew Hirschtritt
Intervention as Prevention? Maybe Not
A core tenet of child psychiatry is the assumption that treating children with mental disorders will help them avoid adult illness. This is “intervention as prevention.” We may need to rethink this assumption as new longitudinal research reports that interventions for children do not reduce the risk of adult mental illness.
The classic Great Smoky Mountain Study began in 11 mostly rural North Carolina counties in 1993 by recruiting 1,420 children from ages 9 to 16. This study has already been a source of important findings about the value of specialty mental health services for children in a “real world” setting. Now, almost 30 years later, William Copeland from the University of Vermont and colleagues are asking whether the benefits of treatment in childhood persist into adulthood.
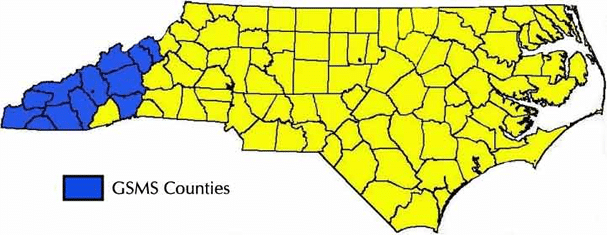
The original participants in GSMS include 1420 children and their parents, from 11 counties in western North Carolina, including 349 youth in the Eastern Band of the Cherokee Nation
The results will surprise those who think of “intervention as prevention.” Receiving treatment, including effective treatment, in childhood did not reduce the subsequent prevalence or severity of psychiatric disorders in adulthood. Even when comparing adults who had been diagnosed with the same disorder in childhood, a history of having received effective treatment did not reduce the subsequent risk of a mental disorder. Moreover, children who received services in childhood were at double the risk for developing adult substance disorders. These surprising and disappointing findings could not be explained by the childhood diagnosis, the amount of treatment, or demographic variables. Apparently, mental disorders in childhood, treated or not, tend to recur as chronic illnesses in adults.
The authors say it best: “The ‘treatment as prevention’ hypothesis is simple, plausible, and a source of hope, but is not supported here. Strategies to reduce the public health burden of mental illness across the lifespan will have to be multi-faceted including prevention programs focused on shared risk factors (e.g., poverty), a service system that addresses [mental health] at each part of the lifespan and across key transitions, and evidence-based community [mental health] services. Such measures may have ‘spillover’ effects that improve cost-effectiveness, but chronic mental health problems like chronic physical health problems may be a recurrent feature of the human experience.”
Does “Real World” Childhood Mental Health Services Reduce Risk for Adult Psychiatric Disorders? Journal of the American Academy of Child and Adolescent Psychiatry, January 18, 2022
-Tom Insel
Digital Markers of Psychosis
In assessing a person with psychosis, clinicians use terms like blunted affect, rapid speech, loose associations, and paranoia. Each of these labels is based on an interview and relies on subjective observation. But what if there were objective, precise, and reproducible markers of psychosis? Several groups have been working on digital assessments of voice, speech, and facial expression to create objective markers that could quantify psychosis the way blood sugar levels monitor diabetes. This week brought two new entries in this quickly expanding field of psychiatric digital phenotyping.
A team led by Tovah Cowan from Louisiana State University explored the construct of “blunted affect” –a reduction in facial expression of emotion. Blunted affect is common in people with serious mental illness, ranging from major depression to bipolar disorder. Cowan and colleagues used computerized analysis of facial expressions of adults with psychosis to identify what clinicians were labeling as blunted affect.
They found that blunted affect was not a single feature. Indeed, patients expressed a range of facial emotions, but when clinicians described someone as having blunted affect, they were responding mostly to decreased expressions of surprise and increases in anger, sadness, and fear – but were missing out on other facial features that only a computer can measure – such as eye blink rate or the duration of a smile. Adding those elements can provide objective, quantifiable data to augment clinical assessments of emotion.
Anzar Abbas of AiCure and colleagues have previously studied facial expression of emotion and vocal markers in people with schizophrenia using computer vision and vocal acoustic analysis. Their laboratory work had previously established a range of vocal measures, such as the loudness of speech and the pitch variability, as components of the “negative symptoms” of schizophrenia (those that relate to a person being socially withdrawn or incommunicative).
In new research, Abbas and colleagues show that both the computer vision of facial expression of emotion and vocal analysis can be collected in a remote clinical interview via a smartphone. These measures correlate with clinical ratings of symptom severity for people diagnosed with schizophrenia. This work suggests that teletherapy could capture rich data in the course of an interview to enhance the assessment of core features of schizophrenia.
Taken together, these two new studies add to a body of work that is changing how clinical scientists study the core symptoms of schizophrenia. The use of objective tools to quantify cognitive and behavioral aspects of psychosis are an important step towards improving diagnostic precision. And more accurate diagnoses may point the way to more effective, patient-specific treatments.
Computerized analysis of facial expressions in serious mental illness Schizophrenia Research, March 1, 2022
Facial and Vocal Markers of Schizophrenia Measured Using Remote Smartphone Assessments: Observational Study JMIR Formative Research. January 21, 2022
-Tom Insel
Many Pregnant Jail Inmates Aren’t Getting Opioid Use Disorder Treatment

Researchers and advocates have long been concerned that pregnant women who are incarcerated in jails across the country don’t get the medical care they need during and after pregnancy. Women make up about 71,000 of the nearly 550,000 inmates confined in jails. Now new research shows that many jails don’t provide pregnant jail inmates with evidence-based treatments for opioid use disorders.
Johns Hopkins physician and researcher Carolyn Sufrin and colleagues surveyed medical and custodial officials at U.S. jails. While most didn’t reply, 29% (836 jails) provided enough information to be included in the study, an equally representative mix metropolitan and rural facilities.
The survey asked whether jails provided evidence-based medications for opioid use disorder (MOUD) – namely methadone and buprenorphine – to pregnant inmates and, if so, under what circumstances. The findings show serious limitations in the availability of these vital medications.
- 3% of all women held in jails on one specific day (6/30/2019) were pregnant.
- 60% of jails had a “high certainty” of having MOUD available at all for pregnant inmates. About a third (31%) offered both buprenorphine and methadone. About one-third (32%) both initiated and continued MOUD while 28% only continued – but didn’t initiate – MOUD. Nearly a quarter of jails (23%) provided MOUD only for opioid withdrawal.
- Among the 504 jails that offered MOUD, only 24% routinely continued MOUD in the postpartum period. The remainder either abruptly or gradually discontinued MOUD after delivery or only continued treatment under specific conditions (e.g., if the inmate was expressing breast milk).
- Jails with higher odds of providing MOUD to pregnant inmates were located in the Northeast (with lower odds in Midwestern and Southern jails), in metropolitan settings, had higher numbers of women inmates, provided pregnancy testing within 2 weeks of booking, and used private health care contractors (in contrast to custodial staff) for care delivery.
These results are especially concerning given the steadily increasing rates of perinatal opioid use. Further, the lack of consistent access to MOUD for pregnant inmates only serves to solidify the association between drug use and incarceration. Providing MOUD to pregnant inmates during and after pregnancy would likely help them abstain from opioid use after release and avoid reincarceration.
Availability of Medications for the Treatment of Opioid Use Disorder Among Pregnant and Postpartum Individuals in US Jails. JAMA Network Open, January 20, 2022.
-Matthew Hirschtritt
Who Are We Really Studying When We Study Schizophrenia?
Every clinical trial specifies who’s eligible – or ineligible – to participate. It’s a well-known research problem that these inclusion and exclusion criteria often end up creating a rarified subset of people who aren’t representative of those who actually have a given disorder in the real world. Now a new Nordic study suggests that the few people with schizophrenia who make it into clinical trials don’t reflect most people living with the disorder.
A research team led by Heidi Taipale of the University of Eastern Finland and the Karolinska Institute examined data of more than 25,000 people with schizophrenia and related disorders from national patient registries in Finland and Sweden. They applied eligibility criteria that are often used in clinical trials to test relapse prevention – things like requiring people to be consistent users of antipsychotic medication or to have had no psychiatric hospitalizations for 12 weeks. Frequently, people may be excluded if they have a history of substance use, a high risk of suicide, have been diagnosed with a serious medical condition, are using an antidepressant or mood stabilizer, or are pregnant. The study team extracted records from people who’d been taking an antipsychotic for at least 12 weeks and traced their mental health service use over the ensuing year.
After applying these kinds of eligibility criteria, the researchers found that 79% of people with schizophrenia and related disorders would’ve been excluded from a hypothetical clinical trial. Serious medical conditions and antidepressant or mood stabilizer use were the top reasons for exclusion. The excluded people were also more likely to be hospitalized for psychosis in the one-year follow-up period than the people who would have made it into the study. The ineligible people were more likely to have failed to improve on multiple antipsychotics, to have had tardive dyskinesia (a side effect of some antipsychotics), and to have attempted suicide. The more ineligibility criteria a person racked up, the more likely she was to be hospitalized.
This report follows in the footsteps of multiple other studies with similar conclusions. For example, studies that use positron emission tomography to examine brain activity in schizophrenia likely recruit people who are younger and less ill than most people with schizophrenia. Overly selective recruitment is a major potential cause of bias in these studies. The challenge for researchers is balancing the need to create relatively homogenous study samples so they can test an intervention without too many confounding variables, with the need to represent the diversity of people in the community who are actually using these treatments.
Representation and Outcomes of Individuals with Schizophrenia Seen in Everyday Practice Who Are Ineligible for Randomized Clinical Trials. JAMA Psychiatry, January 26, 2022.
-Matthew Hirschtritt
If you or anyone you know is considering suicide, call the National Suicide Prevention Lifeline at 1-800-273-8255. And if you’re a veteran, press 1.
Tom Insel, MD, is a psychiatrist, neuroscientist, and former director of the National Institute of Mental Health (NIMH). He is a donor to MindSite News and chair of its Editorial Advisory Board. Dr. Insel’s financial conflict of interest statement, which includes equity and advisory roles in several early-stage mental health technology companies, can be found here.
Matthew Hirschtritt, MD, MPH, is a clinical psychiatrist with the Permanente Medical Group, Inc., a mental health services researcher with the Division of Research, Kaiser Permanente Northern California, and assistant program director of the Kaiser Permanente Oakland Adult Psychiatry Training Program. His current research focuses on identification and treatment of patients with first-episode psychosis, as well as implementation of a telehealth-based mental health evaluation and referral program.
Biden Admin Takes on Insurers Over Mental Health
Biden administration begins effort to compel U.S. health insurers to equitably pay for mental health services.
Black-Owned Hospice Brings Ease in Dying to Black Families
A Nashville hospice agency focuses on increasing use of end-of-life care by Black families.
The name “MindSite News” is used with the express permission of Mindsight Institute, an educational organization offering online learning and in-person workshops in the field of mental health and wellbeing. MindSite News and Mindsight Institute are separate, unaffiliated entities that are aligned in making science accessible and promoting mental health globally.