Covid’s impact on mental health
Covid-19’s long-term mental health effects, a surprising finding about suicide prevention and the impact of Housing First.

It’s been a week of intense activity in the mental health world. The launch of the Lancet Commission on Depression, the release of Inseparable’s report card on school mental health, hearings on the Hill, and yes, some pretty interesting science as well. This week we review studies on the long-term mental health effects of Covid-19, a surprising finding about suicide prevention, a new discovery on how your gut affects your brain, and the long-term impact of Housing First. Let us know what we missed. We’d love to hear from you.
MindSite Daily News is taking a day off on Monday for President’s Day but we’ll be back on Tuesday. Have a great long weekend. Read on!
Housing First But Not Last
Nearly every discussion about serious mental illness where I live in the Bay Area includes a conversation about homelessness. Whether as a cause or consequence of mental illness, homelessness has become the topic that dominates political and social discourse, especially during the pandemic. So, I was intrigued to see a new report on a randomized clinical trial of Housing First, not in San Francisco or LA, but in four cities in France.

S. Loubiere and colleagues in Marseille followed 703 people with schizophrenia or bipolar disorder who were homeless or precariously housed. Half the group got Housing First – immediate access to housing, along with support from a team providing assertive community treatment, a form of intensive case management. The other half got standard support and services available generally in the community. After a two-year follow-up showed reductions in symptoms and hospitalization for those in the Housing First group, the French government scaled up Housing First nationwide in 2017.
After four years, the story is much the same. While the groups do not differ in many measures of recovery, such as “personal confidence and hope” or “goal and success orientation,” the Housing First group spent substantially more days in independent housing, fewer days in the hospital, and reported a greater sense of autonomy. One surprise: the Housing First group was more likely to report alcohol abuse or addiction, but the authors attribute this to a reporting bias since participants in the treatment-as-usual group could lose services if they admitted to alcohol problems.
What I find surprising with the French experience is that Housing First impacts independence and hospitalization but doesn’t seem to confer better clinical results. People in the Housing First group were no more likely to be in remission and it is not clear from this study how many of the participants were employed or thriving in a social network.
Housing is a vital part of the treatment plan for people with serious mental illness, but it is not yet baked into health care. Providers in most states cannot write a prescription for safe housing. Combining housing with Assertive Community Treatment, as done with Housing First, can be a foundation for recovery. Housing may come first, but it is only part of a series of interventions needed for recovery.
Housing First for homeless people with severe mental illness: extended 4-year follow-up and analysis of recovery and housing stability from the randomized Un Chez Soi d’Abord trial. Epidemiology and Psychiatric Services, February 5, 2022.
– Tom Insel
Covid-19’s Long Tail

Covid-19 has been bad for our mental health. That’s not news. But a new study of over 150,000 patients in the VA health care system shows that the mental health consequences of Covid-19 linger much longer than the acute syndrome.
The study, led by Ziyad Al-Aly of the Clinical Epidemiology Center at the VA Saint Louis Health Care System, captured people who were infected during the first 10 months of the pandemic, then checked back a year later to look for new mental health diagnoses. Compared with people who didn’t get infected, those who did were 35% to 39% more likely to have a new anxiety disorder, depressive disorder, or stress-adjustment disorder. In addition, the use of antidepressants, benzodiazepines, and opiates increased in the year after a Covid-19 infection. The biggest effects were in cognitive decline and sleep disorder. Among people who got infected, the risk of cognitive decline was 80% greater and the risk of having a sleep disorder was 41% greater a year post-Covid, compared with those never infected.
It’s possible that similar effects would emerge after any serious infectious disease. But the risk of mental health disorders was consistently higher in the Covid-19 group compared to people with seasonal influenza. The mental health consequences were also higher among those admitted to the hospital with covid-19 versus those admitted to the hospital with seasonal influenza or for any other cause.
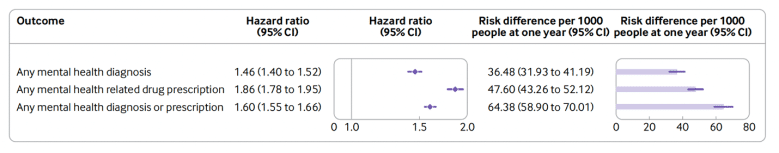
These results, the first showing long-term mental health effects of Covid-19 infection, suggest we may be just beginning to glimpse the mental health impact of this pandemic. The social isolation, loss, uncertainty, and general stress have been bad for mental health in the entire population. These new findings suggest that the virus itself may cause neuropsychiatric effects that will linger, compounding all these other effects.
Risks of mental health outcomes in people with covid-19: cohort study British Medical Journal Feb 16, 2022
-Tom Insel
You Are What You Eat
It’s a familiar scenario for many: You’re about to speak to a roomful of strangers, take a high-stakes test, or have a difficult conversation – and suddenly you feel like your stomach is twisting in knots. For those with irritable bowel syndrome – chronic gastrointestinal issues like diarrhea and constipation, without a clear physical cause – this pattern leads to considerable distress. But the brain-gut connection also goes in the opposite direction, with signals from the gut driving how well we think and our emotions.
Now a new study shows that mice with high levels of a microbial by-product in their gut appear more anxious – and there may be a neurobiological explanation.
Caltech researcher Brittany Needham, a postdoc in the research group of Sarkis Mazmanian, and colleagues used a mouse model to study the association between the presence of a bacterial metabolite called 4-ethylphenyl sulfate (4EPS) and anxiety-like symptoms. 4EPS is produced by intestinal microbes and is then absorbed and distributed in the bloodstream. The Mazmanian lab had already shown in a previous mouse study that high levels of 4EPS were associated with autism-like symptoms; cleaning the blood of 4EPS decreased these symptoms. More recently, this same group demonstrated that children with autism spectrum disorders had substantially higher levels of 4EPS compared with typically developing children.
In the current study, Needham and colleagues compared two groups of mice: One group was fed bacteria that produced 4EPS and a comparison group was fed similar bacteria that couldn’t produce 4EPS. They exposed both mouse groups to conditions that tend to increase mouse “anxiety.” The high-4EPS mice spent more time hiding and less time exploring compared with the other mice. Brain images showed that areas and circuits associated with anxiety were more active in the high-4EPS mice. Further, when researchers dissected their brain cells, the high-4EPS mice had less myelin coating their nerve fibers, decreasing the insulation that protects delicate nerve fibers.
When the high-4EPS mice were treated with a chemical that increases myelin production, normal myelin production was restored, and the mice appeared less anxious. In a related paper published at the same time in Nature Medicine, the Mazmanian group showed that administering a drug that cuts levels of 4EPS and other metabolites also decreased anxiety and irritability among a small group of youth with autism spectrum disorder.
Though these results are intriguing, many questions remain: Does 4EPS directly acts on brain cells, or are there unmeasured, intermediary steps? Why might decreased myelin production lead to higher levels of anxiety? And are there other microbacterial byproducts associated with anxiety in the gut, especially in humans?
Still, this study adds weight to an old adage: You are what you eat. Or nibble.
A gut-derived metabolite alters brain activity and anxiety behaviour in mice. Nature, February 14, 2022
─ Matthew Hirschtritt
We’re Going to Need a Bigger Boat

The late Jerome Motto, a psychiatrist in San Francisco, famously claimed he could prevent suicides by sending a postcard to his patients every month after an attempt. This idea, part of what we now call postvention, gained some support with a randomized controlled trial showing a 50% reduction in subsequent suicide attempts using the postcard intervention. Although other studies were less supportive, the idea that light touch interventions can prevent suicide has an undeniable appeal.
Given that appeal, new results from a large-scale study are sobering. Gregory E. Simon from Kaiser Permanente Research Institute in Seattle and colleagues investigated the effects of two low-intensity interventions versus usual care to prevent suicide in over 18,000 patients who had frequent suicidal thoughts. One involved care management with regular outreach; the other involved training in four dialectical behavior therapy (DBT) skills. These interventions were delivered through electronic messages between patients and their clinical team. Usual care consisted of ongoing mental health care without the care management or skills training.
Up to 18 months later, 540 participants had engaged in some form of self-harm. Surprisingly, there were no large differences between the treatment groups and there was a slightly higher risk of self-harm among those trained in DBT skills than in those getting usual care. These low-intensity interventions may be scalable and practical, but at first glance they don’t seem to reduce suicide.
However, a closer look reveals important caveats, some of which were noted in an accompanying editorial. Engagement was low and drop-outs were high: In the intervention arms, 44% of the sample dropped out after three months. While DBT has been widely promoted as a psychological intervention for suicidal ideation, there is more to DBT than remote training on four skills. Therapeutic alliance and social support are important parts of the model that may not work well with a remote, low-intensity intervention.
But this large study in a real-world setting using scalable interventions does make one point clearly. Reducing suicide is difficult. Online CBT seems to help with depression and anxiety; one might have thought that online assistance would also help prevent self-harm in people with suicidal ideation. But apparently not. As Chief Brody said in Jaws, “We’re going to need a bigger boat.”
Effect of Offering Care Management or Online Dialectical Behavior Therapy Skills Training vs Usual Care on Self-harm Among Adult Outpatients With Suicidal Ideation: A Randomized Clinical Trial JAMA, February 15, 2022.
– Tom Insel
If you or anyone you know is considering suicide, call the National Suicide Prevention Lifeline at 1-800-273-8255. And if you’re a veteran, press 1.
Tom Insel, MD, is a psychiatrist, neuroscientist, and former director of the National Institute of Mental Health (NIMH). He is a donor to MindSite News and chair of its Editorial Advisory Board. Dr. Insel’s financial conflict of interest statement, which includes equity and advisory roles in several early-stage mental health technology companies, can be found here.
Matthew Hirschtritt, MD, MPH, is a clinical psychiatrist with the Permanente Medical Group, Inc., a mental health services researcher with the Division of Research, Kaiser Permanente Northern California, and assistant program director of the Kaiser Permanente Oakland Adult Psychiatry Training Program. His current research focuses on identification and treatment of patients with first-episode psychosis, as well as implementation of a telehealth-based mental health evaluation and referral program.
The name “MindSite News” is used with the express permission of Mindsight Institute, an educational organization offering online learning and in-person workshops in the field of mental health and wellbeing. MindSite News and Mindsight Institute are separate, unaffiliated entities that are aligned in making science accessible and promoting mental health globally.








