Heatwaves and Mental Health
New research demonstrates how high temperatures can negatively impact mental health and increase emergency room visits.

This week’s Research Roundup arrives after so many unsettling stories in the wider world, with the death of our colleague Paul Farmer an especially painful loss. Paul was unique in the global health world, pointing us not only to the social determinants of health but the moral determinants of health. As he said in his last book, To Repair the World, “This growing outcome gap is related to the growing income gap.”

Whether in Haiti or Rwanda or Boston, Paul practiced what he preached. He liked to use the term “accompaniment” when talking about health care, meaning that we must literally “break bread with” those we serve. His death was completely unexpected. I received a cheery email from him from Rwanda just a few days ago. Without Paul’s “accompaniment,” our world is truly a lesser place. –Tom Insel
It’s Getting Hot in Here

Climate change negatively impacts mental health. Flooding, droughts, extreme heat, wildfires and worsened air quality have been associated with increased rates of anxiety, depression, PTSD and even aggression. Extreme heat has been linked with increased irritability, depressive symptoms, suicide, domestic violence and substance abuse. Now, new research demonstrates how high temperatures can specifically impact emergency department mental health visits.
Amruta Nori-Sarma of the Boston University School of Public Health and colleagues mined a large database of 2.2 million commercially insured adults in the U.S. to track reasons for 3.5 million emergency department visits from 2010 through 2019. They found that during periods of “extreme heat” – defined as being in the top 5 percentile of historic temperatures for a local area – there was an 8% increase in visits with a mental health diagnosis, compared with cooler days.
The associations between extreme heat days and mental health-related ED visits were higher for men than for women, and among visits in the Northeast, Midwest, and Northwest.
As heat waves increase, the U.S. needs to prepare not only for the immediate physical hazards of high temperatures but also the impact on Americans’ mental health. Though not directly addressed in this study, the people most impacted by extreme heat may also face other challenges, like insecure housing, serious mental illness, and poverty. This study provides yet another data point for the enormous need to address climate change and ensure health equity at the same time.
Association Between Ambient Heat and Risk of Emergency Department Visits for Mental Health Among US Adults, 2010 to 2019 JAMA Psychiatry, February 23, 2022.
– Matthew Hirschtritt
The Engagement Challenge for Early Psychosis

When a young person in the U.S. experiences a first episode of psychosis, it typically takes 74 weeks – almost a year and half – for them to receive treatment. Plenty of research shows that treating people earlier in an episode reduces the damage from the psychotic experience and confers a better outcome. With a goal of screening for mental illness, Mental Health America in 2015 began offering online, anonymous screening tests to the general public for a range of mental health conditions.
One screening questionnaire specifically asked about psychotic symptoms. In 2017, over 120,000 people completed this psychosis questionnaire. Now a team of researchers at the University of California, Davis, has analyzed the results of those responses. Roughly 80% of those taking the psychosis test reported they were experiencing symptoms and distress significant enough to merit referral to a mental health specialist. Only half of these had previously received a psychiatric diagnosis.
What did these people plan to do for their mental health? Mostly, they planned to seek more information, either from a family member, friend, or professional or from an online source. Nearly 30% reported that they did not plan any further action, and only 17% said they would seek treatment. Respondents who self-identified as African American were more likely to report a willingness to seek treatment.
Online, anonymous questionnaires without follow-up or clinical validation are subject to a range of inaccuracies, from false reports to redundant entries. But Mental Health America has looked carefully at the pattern of responses, providing some assurance that their overall conclusion is solid: Most young people with significant distress from psychotic-like experiences are not planning to seek treatment at the time when treatment might be most effective. The implication is clear. If we want better outcomes, we need to understand how, where, and when to engage young people in care.
Online Psychosis Screening: Characterizing an Underexamined Population to Improve Access and Equity, Psychiatric Services, Feb 17, 2022
– Tom Insel
Sobering News on Alcohol Treatment Rates

Alcohol use disorder remains a serious problem in the U.S., killing 95,000 people a year, and several reports have suggested that alcohol sales and use increased during the COVID-19 pandemic. Yet data from an annual survey suggests that even before the pandemic, the rate of people receiving treatment for an alcohol disorder was not keeping pace – and had fallen significantly during the preceding decade.
The National Survey on Drug Use and Health has been collecting self-reported drug and alcohol use data from Americans ages 12 and older since 1979 and is designed to be representative of the non-institutionalized U.S. population. Aidan Larsen of Mathematica Policy Research and colleagues used several waves of the survey data to examine trends in alcohol treatment among adults aged 18 to 64.
Larsen’s team identified nearly 37,000 non-elderly adults with an alcohol disorder from three combined waves of the annual survey: 2008-2010, 2011-2013, and 2014-2017. In each period, the researchers calculated how many of these adults received treatment in a medical setting like a rehab center, doctor’s office or the emergency department; got assistance through self-help groups; or got no treatment at all.
Their findings: Rates of treatment decreased from 6.9% in 2008-2010 to 5.8% in 2014-2017. What’s most striking here is the low rates of alcohol treatment at all time points.
Our understanding of the grave costs of unhealthy alcohol use has increased in recent years, so why have treatment rates been dropping – even before the pandemic? The researchers surmise that one explanation may lurk in escalating out-of-pocket costs for substance-use treatments over the past several years.
Regardless of the explanation, these results are sobering. More work needs to be done to consistently screen for alcohol disorders and unhealthy alcohol use and to ensure that people needing treatment can obtain – and get reimbursed for – empirically based, affordable, and accessible treatment.
Trends in Alcohol Use Disorder Treatment Utilization and Setting From 2008 to 2017 Psychiatric Services, February 23, 2022.
– Matthew Hirschtritt
The Pandemic’s Outsized Toll on Young Women with Eating Disorders
It’s estimated that about 9% of Americans – or about 28.8 million people – will experience an eating disorder in their lifetime. Eating disorders all share an unhealthy relationship with food, but manifest in various ways, ranging from anorexia nervosa to binge-eating disorder. The stressors of the COVID-19 pandemic have posed special challenges for people with eating disorders and new research shows just how profound the pandemic’s impact has been.
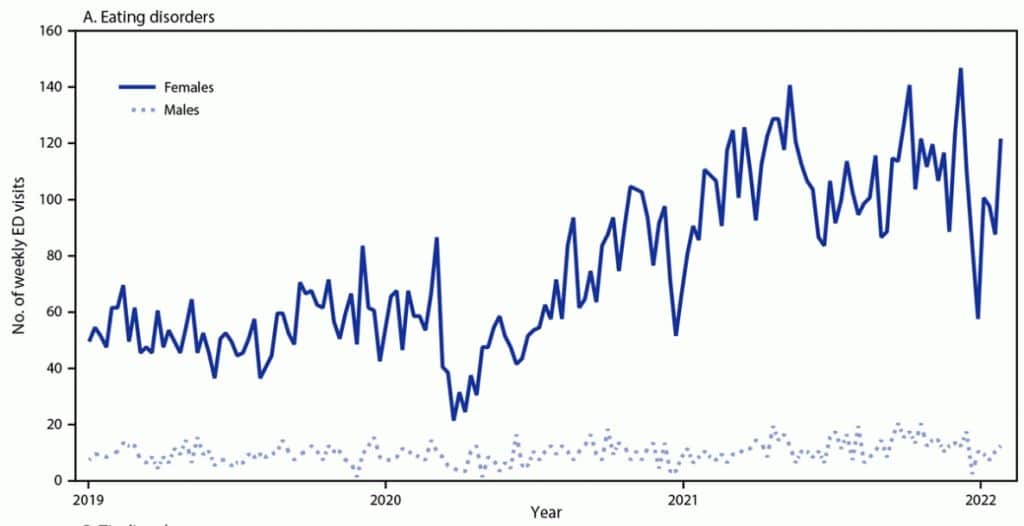
Lakshmi Radhakrishnan of the CDC and colleagues used data from the National Syndromic Surveillance Program to examine emergency department (ED) visits among youth ages 0 to 17 years in three evenly spaced periods between March 2020 and January 2022. While overall emergency visits for mental health conditions decreased during the pandemic compared to 2019, weekly ED visits for eating disorders among females aged 12 to 17 increased in each of the three pandemic periods compared with the previous year. Overall, the proportion of visits by teenage girls to emergency departments that were for eating disorders nearly doubled.
A separate study conducted earlier in the pandemic by a team of US- and UK-based researchers led by Maxime Taquet of the University of Oxford and Oxford Health NHS Foundation Trust found a similar increase in eating disorders. Using aggregated electronic health record data of nearly 81 million patients, mostly in the U.S., they found a 15.3% increase in eating disorder diagnoses in the 2020-2021 period compared with the previous year. This increased incidence was limited to females, was greatest for youth ages 10 to 19 and was predominantly driven by people with anorexia nervosa. Even more concerning, youth with eating disorders were about 69% more likely to have attempted suicide and 30% more likely to report suicidal thoughts during the pandemic, compared with the prior three years.
Taken together, these studies highlight the toll the pandemic has taken among young people, especially women, with eating disorders. Why such a steep increase? The answer is not provided in these studies but the combined stress of social isolation, drastically changed physical activity patterns, and family-related tensions have probably contributed. We need a greater understanding of youth who are especially vulnerable to eating disorders and may face specific challenges, including those who are LGBTQ+. We need to do better screening for eating disorders and offer resources and treatment more quickly to young people dealing with these disabling conditions.
Pediatric Emergency Department Visits Associated with Mental Health Conditions Before and During the COVID-19 Pandemic — United States, January 2019–January 2022 Morbidity and Mortality Weekly Report, February 18, 2022.
Incidence and outcomes of eating disorders during the COVID-19 pandemic The British Journal of Psychiatry, July 27, 2021.
– Matthew Hirschtritt
If you or anyone you know is considering suicide, call the National Suicide Prevention Lifeline at 1-800-273-8255. And if you’re a veteran, press 1.
Tom Insel, MD, is a psychiatrist, neuroscientist, and former director of the National Institute of Mental Health (NIMH). He is a donor to MindSite News and chair of its Editorial Advisory Board. Dr. Insel’s financial conflict of interest statement, which includes equity and advisory roles in several early-stage mental health technology companies, can be found here.
Matthew Hirschtritt, MD, MPH, is a clinical psychiatrist with the Permanente Medical Group, Inc., a mental health services researcher with the Division of Research, Kaiser Permanente Northern California, and assistant program director of the Kaiser Permanente Oakland Adult Psychiatry Training Program. His current research focuses on identification and treatment of patients with first-episode psychosis, as well as implementation of a telehealth-based mental health evaluation and referral program.
The name “MindSite News” is used with the express permission of Mindsight Institute, an educational organization offering online learning and in-person workshops in the field of mental health and wellbeing. MindSite News and Mindsight Institute are separate, unaffiliated entities that are aligned in making science accessible and promoting mental health globally.