Death rates increased the most during pandemic for people with mental illness and brain disorders, Medicare data shows
The death rate for people with schizophrenia increased more than any other group during the pandemic, along with many excess deaths from other mental illnesses and brain-related disorders.

The death rate for people with schizophrenia increased far more than it did for any other group early in the pandemic, according to a new analysis of Medicare statistics. Excess deaths for those with bipolar and post-traumatic stress disorders weren’t far behind, along with other brain-related conditions like autism, intellectual disability and Alzheimer’s disease.

Mortality rates among patients with pulmonary disorders and the deadliest cancers, who were repeatedly warned that Covid-19 posed a very high risk, increased less than the average for all Medicare beneficiaries in 2020. The lung cancer death rate actually dropped below the pre-pandemic level in 2021.
Researchers at NORC at the University of Chicago said this was the biggest surprise in their data analysis. They attributed the finding to the medical community’s concerted efforts to protect its most vulnerable patients – with implications for improvement in future pandemics.
People with cancer also generally live at home rather than in institutional settings where the coronavirus spread like wildfire – and where those with serious mental illness and brain-related disorders more often reside.
Extremely high increases in death rates were most apparent “among conditions that affect cognition,” said Alex Hartzman, director of health care analytics, in an email. People with impaired cognitive abilities are more likely to require caregivers, who can transmit the virus regardless of setting, and less likely to follow public health precautions.
Caroline Pearson, senior vice president for health care at NORC, told MindSite News that she had expected caregiving to be a major driver of mortality but “was really shocked at how much.”
Mortality for a group of conditions that are likely to require professional caregiving increased by 21.5% from 2019, before the pandemic, to 2020, compared to a 15.1% increase among all Medicare beneficiaries. The percent difference between expected (normal) and actual death rates is known as excess mortality. The NORC data included deaths from all causes, not just Covid-19, and has yet to be peer-reviewed.
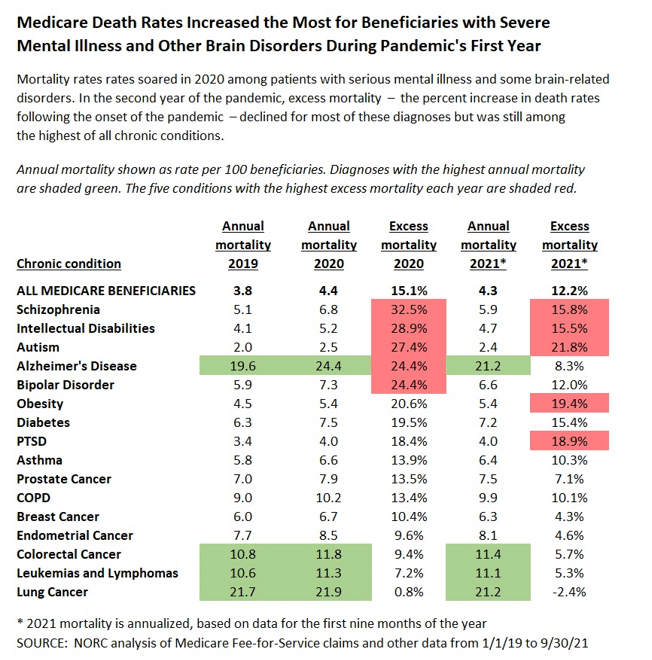
Excess mortality dropped significantly for most of the caregiver-intensive conditions during the pandemic’s second year, although it remained far higher than before Covid. Pearson said that the availability of vaccines almost certainly explained the 2021 drop. Elderly people rushed to get the newly available shots and many nursing homes, overwhelmed by deaths the first year, quickly vaccinated their residents.
The impact was stark. Excess mortality for schizophrenia was a staggering 32.5% in 2020 but fell by more than half, to 15.8%, the next year – presumably due largely to vaccination, but so many deaths the first year also meant that the population remaining in 2021 was slightly healthier.
PTSD was the only diagnosis among 18 chronic conditions that normally have the highest death rates to see even higher excess mortality the second year. Pearson speculated that people with PTSD may be somewhat less likely to live in congregate care settings than those with other serious mental health conditions, and perhaps were less likely to get vaccinated.
Mental illness, Alzheimer’s and institutional living have long been linked. “There is likely a fair amount of overlap between the severe psychiatric disorders and dementia within the Medicare population,” said Mark Olfson, a professor of psychiatry and epidemiology at Columbia University, who found in a pre-pandemic study published last year that 28% of adult Medicare beneficiaries with schizophrenia had dementia by age 66 and 70% by age 80.
People with serious mental illness also have a lot of chronic conditions. NORC did not examine numbers of conditions linked to specific diagnoses, but it found that Medicare beneficiaries who died in 2020 had an average of 12.2 chronic conditions compared to 6.6 for the entire Medicare population.
An Olfson study several years ago of adults in the Medicaid program found that schizophrenics were 10 times more likely to die of chronic obstructive pulmonary disease than the general population. “Beyond COPD, patients with schizophrenia have elevated rates of obesity, diabetes, cardiovascular disease, and other persistent medical conditions that increase their risk of mortality during the Covid era,” he said in an email.
They also may have difficulty recognizing signs and symptoms of Covid, navigating the health care system and communicating with their physicians.
Pearson, who interviewed operators of memory care facilities for unrelated research, said they told her that they couldn’t get their dementia patients to follow pandemic guidelines. Mentally ill patients frequently were “afraid of masks,” she heard, both their own and those worn by caregivers. Even when a staff member they knew well came into the room with a mask on, “it really terrified those patients,” she said.
This vulnerability of people with severe mental illness to infectious diseases was well-known in the medical community and psychiatric hospitals have historically been associated with outbreaks of viral infections, Olfson said.
“There should have been a strong presumption that this was a vulnerable group and appropriate public health and clinical precautions should have been taken,” Olfson said. Were such precautions taken? He couldn’t say, but his general sense was that health care systems were overwhelmed early on and “little attention was devoted to the specific Covid-related vulnerabilities of people with severe mental illnesses and other marginalized groups.”
Dozens of organizations representing people with disabilities vented their frustration over similar issues and many others in a January letter to Rochelle Walensky, director of the Centers for Disease Control and Prevention. They quickly got a meeting and presented recommendations for improvement.
The experts at NORC found implications for the nation’s response to future pandemics in their most surprising findings.
“Nursing homes and in-home caregivers need clear plans in place to quickly change the way they provide care to decrease the risk of transmissible infections and implement those plans at the earliest stages of a new outbreak,” Pearson said. “The health system needs to draw lessons from how patients with cancers and pulmonary diseases were cared for given their low excess death rates.”
The name “MindSite News” is used with the express permission of Mindsight Institute, an educational organization offering online learning and in-person workshops in the field of mental health and wellbeing. MindSite News and Mindsight Institute are separate, unaffiliated entities that are aligned in making science accessible and promoting mental health globally.